Contents
hide
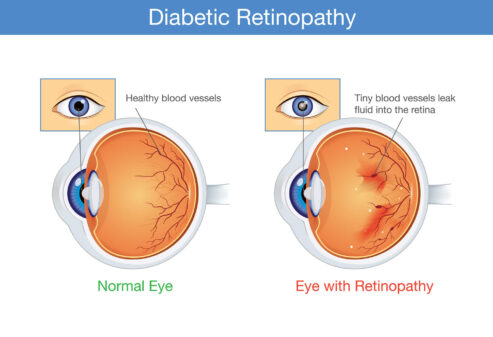
Diabetic retinopathy is an eye disease that happens when diabetes damages the blood vessels in the retina. The retina is the part of the eye that senses light and helps you see. Diabetic retinopathy is a major cause of vision loss and blindness. Early detection and proper care can help prevent vision loss.
This guide explains what diabetic retinopathy is, how it develops, the stages and symptoms, and the treatments that are available. It also covers what you can do to protect your vision.
What Is Diabetic Retinopathy?
Diabetic retinopathy is an eye disease caused by diabetes. High blood sugar can damage the small blood vessels in the retina. The retina is the thin layer of tissue in the back of the eye that helps you see.
Over time, these damaged vessels may:
- Leak fluid or blood
- Become blocked
- Grow abnormally
- This can cause the retina to swell or pull away from the back of the eye.
Without treatment, diabetic retinopathy can lead to permanent vision loss or blindness.
Types of Diabetic Retinopathy
There are two main types of diabetic retinopathy. These types show how the disease can get worse over time.
1. Non-Proliferative Diabetic Retinopathy (NPDR)
Non-proliferative diabetic retinopathy is the early stage of the disease. It is also the most common type.
- Small retinal blood vessels weaken.
- Tiny bulges called microaneurysms may form in the blood vessels.
- Mild leakage may occur.
- Often, there are no noticeable symptoms at this stage.
Most people do not know they have diabetic retinopathy at this stage.
2. Proliferative Diabetic Retinopathy (PDR)
This stage is more serious and can cause vision loss.
- New, abnormal blood vessels begin to grow on the surface of the retina. This process is called neovascularization.
- These new blood vessels are weak and can bleed into the vitreous. The vitreous is the clear gel that fills the inside of the eye.
- Scar tissue can also form because of this abnormal blood vessel growth.
- The risk of the retina pulling away from the back of the eye goes up during this stage.
If not treated quickly, proliferative diabetic retinopathy can cause sudden and severe vision loss.
The 4 Stages of Diabetic Retinopathy
Diabetic retinopathy is an eye disease that worsens over time if left untreated. It has four stages, from mild changes in the retina to serious problems that can threaten your vision.
Knowing about these stages shows why early detection and regular eye exams are important.
➤ Stage 1: Mild Non-Proliferative Diabetic Retinopathy
(Early Stage – Often Asymptomatic)
This is the first and most common stage of diabetic retinopathy.
What happens:
Tiny bulges called microaneurysms form in the retinal blood vessels.
These vessels may begin to leak small amounts of fluid or blood.
The retina may have mild swelling.
Symptoms:
Usually, there are no symptoms you can notice.
Your vision usually stays normal.
Why is this stage dangerous?
Because there are no warning signs, most people do not know they have damage to the retina. Without regular eye exams, the disease can get worse without you knowing.
What doctors do:
Monitor with annual dilated eye exams.
Your doctor will recommend keeping your blood sugar under good control.
Most people do not need treatment at this stage.
This stage gives you the best chance to stop the disease from getting worse.
➤ Stage 2: Moderate Non-Proliferative Diabetic Retinopathy
(Intermediate Stage)
At this stage, damage to the retinal blood vessels is easier to see.
What happens:
Blood vessels become blocked.
Some parts of the retina get less blood.
Retinal swelling may increase.
Swelling in the center of the retina, called macular edema, may start to appear.
Possible symptoms:
You may have mild blurred vision.
It may be hard to focus your eyes.
Your vision may change over time.
Risks:
There is a higher chance the disease will get worse.
Parts of the retina may not get enough oxygen.
Management:
- You may need eye exams more often.
- Better control of your diabetes is important.
- Your doctor will examine for swelling in the center of your retina.
- You may need early treatment if swelling starts.
This stage is a warning that the disease is getting worse.
➤ Stage 3: Severe Non-Proliferative Diabetic Retinopathy
(Advanced Pre-Proliferative Stage)
This stage is a key point in treating diabetic retinopathy.
What happens:
Many retinal blood vessels become blocked.
Large areas of the retina lose oxygen (ischemia)
The retina releases chemicals that stimulate the growth of new blood vessels.
There is a high risk that the disease will move to the next stage.
Symptoms:
You may notice changes in your vision.
You may see dark or blurry spots.
It may be harder to see at night.
Reading may become more difficult.
Why is this stage dangerous:
The eye begins informing the body to grow new blood vessels — a process that leads to the most severe form of diabetic retinopathy.
Medical management:
- Your doctor will monitor your eyes very closely.
- You may have special eye tests, such as OCT or angiography.
- Possible early laser or injection therapy
- It is important to keep your diabetes and blood pressure under good control.
Without treatment, the disease is very likely to get worse.
➤ Stage 4: Proliferative Diabetic Retinopathy (PDR)
(Advanced & Vision-Threatening Stage)
This is the most serious stage of diabetic retinopathy. It is a major cause of blindness.
What happens:
New, weak blood vessels grow on the retina.
These blood vessels can bleed easily into the clear gel inside the eye.
Scar tissue can form on the retina.
The retina may pull away from the back of the eye.
The pressure inside the eye may go up.
Symptoms:
You may lose vision suddenly.
You may see dark floaters or shapes that resemble cobwebs.
Your vision may be blurry or look distorted.
You may see flashes of light.
You may lose part or all of your vision.
Treatment options:
- You may get anti-VEGF injections. This is often the first treatment doctors use.
- Laser treatment may be used to seal leaking blood vessels.
- Some people may need surgery to remove blood from inside the eye. This is called a vitrectomy.
- Doctors can also treat the retina if it pulls away from the back of the eye.
This stage is a medical emergency. You need care right away.
Summary Table: The 4 Stages of Diabetic Retinopathy
| Stage | Retinal Changes | Symptoms | Treatment |
| Mild NPDR | Microaneurysms | None | Monitoring |
| Moderate NPDR | Vessel blockage | Mild blur | Monitoring |
| Severe NPDR | Retinal ischemia | Vision changes | Close follow-up |
| PDR | New vessels, bleeding | Vision loss | Injections / Surgery |
What Causes Diabetic Retinopathy?
The main cause of diabetic retinopathy is high blood sugar over a long period of time.
High glucose levels:
- High blood sugar can damage the retinal blood vessels.
- This damage can lower the amount of oxygen the retina gets.
- Trigger abnormal vessel growth.
- Cause swelling and bleeding.
Over time, this damage accumulates, leading to vision loss.
Who Is at Risk?
Anyone with diabetes can get diabetic retinopathy. The risk is higher if you have:
- Long duration of diabetes
- Poor blood sugar control
- High blood pressure
- High cholesterol
- Pregnancy
- Kidney disease
- Smoking
- Lack of regular eye exams
The longer you have diabetes, the higher your risk of getting diabetic retinopathy.
Symptoms of Diabetic Retinopathy
In the early stages, you may not have any symptoms.
As diabetic retinopathy gets worse, you may notice:
- Blurred or distorted vision
- Floaters or dark spots
- Difficulty seeing at night
- Fluctuating vision
- Loss of central or peripheral vision
- Dark or empty areas in vision
- Sudden vision loss (advanced cases)
Vision loss from diabetic retinopathy can happen suddenly. It usually does not cause pain.
How Is Diabetic Retinopathy Diagnosed?
Doctors can find diabetic retinopathy with a full eye exam, even before you have symptoms. Finding the disease early is the best way to prevent vision loss.
Common Diagnostic Tests Include:
🔹 Dilated Eye Exam
The doctor will use eye drops to dilate your pupils. This helps the doctor look at the retina for damaged blood vessels, swelling, or bleeding.
The doctor will use eye drops to dilate your pupils. This helps the doctor look at the retina for damaged blood vessels, swelling, or bleeding.
🔹 Optical Coherence Tomography (OCT)
OCT is a painless test that takes detailed pictures of the retina. It helps the doctor find swelling and see how the disease is changing.
OCT is a painless test that takes detailed pictures of the retina. It helps the doctor find swelling and see how the disease is changing.
🔹 Fundus Photography
The doctor may take pictures of your retina to look for changes over time.
The doctor may take pictures of your retina to look for changes over time.
🔹 Fluorescein Angiography
A dye is put into your blood to help the doctor see leaking or blocked blood vessels in the retina. This test is usually done if the disease is more advanced.
A dye is put into your blood to help the doctor see leaking or blocked blood vessels in the retina. This test is usually done if the disease is more advanced.
🔹 Visual Acuity Test
This test checks how well you can see. It helps the doctor detect vision loss caused by retinal damage.
This test checks how well you can see. It helps the doctor detect vision loss caused by retinal damage.
Why Early Diagnosis Matters
Diabetic retinopathy often starts without pain or early warning signs.
By the time you notice changes in your vision:
- Damage may already be advanced.
- Treatment becomes more complex.
- Vision loss may be irreversible.
Finding diabetic retinopathy early means you can get treatment before the damage is permanent.
Recommended Screening Frequency for Diabetic Retinopathy.
| Patient Type | Recommended Eye Exam |
| Type 1 Diabetes | 5 years after diagnosis, then yearly |
| Type 2 Diabetes | At diagnosis, then yearly |
| Pregnant women with diabetes | Before pregnancy & during pregnancy |
| Known retinopathy | Every 3–6 months |
Treatment Options for Diabetic Retinopathy
The treatment you need depends on how advanced your diabetic retinopathy is.
✔ Early-Stage Treatment
- It is important to keep your blood sugar in your target range.
- Managing your blood pressure can help protect your eyes.
- It is also important to keep your cholesterol at a healthy level.
- You need regular eye exams to detect any changes.
✔ Advanced Treatment Options
🔹 Anti-VEGF Injections
- These injections help stop new, abnormal blood vessels from growing in your eye.
- They can help improve your vision or stabilize it.
- This is the most common treatment for advanced diabetic retinopathy.
🔹 Laser Therapy (Photocoagulation)
Laser treatment seals leaking blood vessels in your retina.
This helps prevent more damage to the retina.
🔹 Vitrectomy Surgery
- This surgery removes blood from the clear gel inside the eye.
- Vitrectomy can also be used to treat retinal detachment.
- Doctors usually do this surgery only for advanced diabetic retinopathy.
Possible Complications
If untreated, diabetic retinopathy can lead to:
- Permanent vision loss
- Macular edema
- Vitreous hemorrhage
- Retinal detachment
- Glaucoma
- Cataracts
These problems can cause permanent vision loss or blindness that cannot be reversed.
Prevention & Management Tips
You can lower your risk of diabetic retinopathy by following these steps:
- Keep your blood sugar within your target range.
- Control your blood pressure and cholesterol levels.
- Exercise regularly, as your doctor recommends.
- Eat a balanced diet that is good for people with diabetes.
- Do not smoke, because smoking can raise your risk of eye problems.
- Go to an eye exam every year.
- Follow your doctor’s advice and treatment plan consistently.
The best way to prevent vision loss from diabetic retinopathy is to find it early.
When Should You See an Eye Doctor?
You should see an eye specialist:
- If you have diabetes, see an eye doctor at least once a year.
- See an eye doctor right away if you notice any of the following:
- Sudden vision loss
- Floaters or flashes
- Blurred or distorted vision
- Dark spots in vision
Getting treatment quickly can help save your vision.
FAQ
Can diabetic retinopathy be reversed?
Early stages may stabilize with good blood sugar control. Advanced stages cannot be reversed, but can be treated.
Does diabetic retinopathy cause blindness?
Yes. It is one of the leading causes of blindness worldwide — but early treatment can prevent vision loss.
Is diabetic retinopathy painful?
No. Most patients feel no pain until vision loss begins.
How often should diabetics get an eye exam?
At least once a year, or more often if recommended by an ophthalmologist.
Final Summary
Diabetic retinopathy is a serious problem caused by diabetes. Much of the vision loss it causes can be prevented. The disease often starts without symptoms and can lead to permanent vision loss if it is not treated.
- Early screening
- Good diabetes control
- Have regular eye exams as your doctor recommends.
- Seek prompt treatment if you notice any changes in your vision.
These steps can help protect your eyesight for life.
If you have diabetes, having an annual eye exam is not optional. It is good for preserving your vision.